
Warts and Verrucas
Evidence-based skin care and professional treatment options.
At odNOVA Aesthetics, I frequently see patients who are frustrated by stubborn warts or verrucas that refuse to clear. These lesions are extremely common and harmless, but they can be uncomfortable, contagious, and cosmetically distressing. Fortunately, both home care and medical treatments can achieve excellent results when applied correctly and consistently.
scroll down
Seborrhoeic keratoses · Skin tags (acrochordons) · Cherry angiomas · Milia · Solar lentigines (age/liver spots) · Warts/Verrucae · Selected benign moles · Small benign fibromas ·
Warts and Verrucas: What they are and where they come from ?
Verrucas (plantar warts) and common warts are caused by infection with the human papillomavirus (HPV) - most often types 1, 2, 4, 27, or 57 (Sterling et al., 2014).
HPV is a DNA virus that infects the epidermis, usually entering through tiny abrasions or pressure points on the hands, knees, or feet.
Once inside, the virus infects basal keratinocytes and triggers excessive cell division, producing a thickened, rough lesion. The visible wart is therefore the result of your body’s own skin response to the virus (Lipke, 2006).

How infection spreads ?
HPV is highly contagious and spreads through direct contact with infected skin or contaminated surfaces. The virus can survive briefly on wet floors, towels, footwear or nail instruments.
You may catch or spread it through:
- Touching an infected area or shared gym equipment.
- Autoinoculation (transferring the virus to another body site by picking or shaving).
- Walking barefoot in public changing rooms or around pools.
Most adults have been exposed to HPV at some stage, but only some develop visible warts. A strong cell-mediated immune response can suppress viral replication before lesions appear (Horn et al., 2005).
About me
My name is Piotr Wojtowicz — a pharmacist-prescriber specialising in cosmetic and aesthetic medicine, currently completing postgraduate studies in dermatology.
I approach every treatment with a balance of science, ethics, and artistry, focusing on results that feel authentic, harmonious, and true to each individual.

Type of warts/ verrucas

(i) common wart (Verruca vulgaris); characterised as discrete, round, skin-colored papillomatous papules are produced by HPV-1, HPV-2, and HPV-4

(ii) wart on the sole of the foot, plantar wart (Verruca plantaris); tender growing myrmecia on the bottom of feet caused by HPV 1 and HPV 2
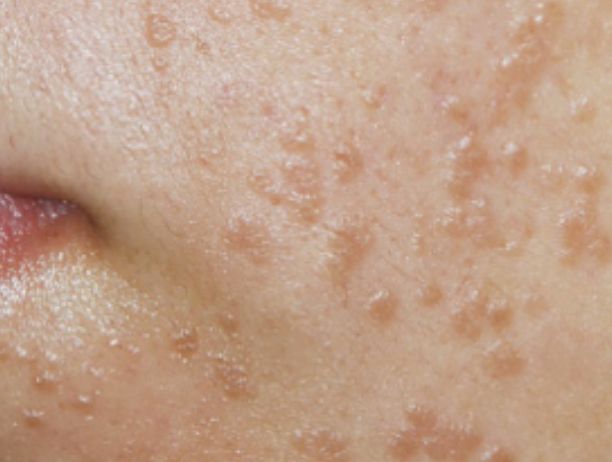
(iii) flat wart or plane wart (Verruca plana) small, flat-topped papules typically 2 to 5 mm reddish-brown or flesh coloured on the face, neck, and the backs of the hands and wrists caused by HPV3 and HPV10

(iv) genital wart (Condyloma accuminatum): flat warts in the anogenital area are usually caused by non-carcinogenic HPV-6 and HPV-11 transmitted through sexual contact.
Understanding and Managing Warts

Why they sometimes persist ?
In most healthy individuals, warts resolve naturally once the immune system recognises the virus.
Around 65 % disappear within two years without treatment (Gibbs et al., 2002).
They can, however, persist longer when:
-
Immunity is reduced (stress, illness, immunosuppressive medication).
-
The area experiences friction or trauma (hands, feet).
-
Skin-picking or nail-biting spreads the infection.
✅ Do:
-
Keep feet covered in communal showers, changing rooms, and pools.
-
Moisturise dry skin to maintain barrier function.
-
Use your own nail and foot tools, and disinfect them regularly.
-
Cover lesions with plasters during sport or gym activity.
-
Wash hands after touching or treating affected areas.
🚫 Avoid:
-
Picking, cutting, or biting warts.
-
Sharing towels, socks or gloves.
-
Walking barefoot on communal floors if you have verrucas.
Good hygiene dramatically reduces spread to others or other areas of your own skin.
Important advice
Ask your pharmacist to recommend a suitable salicylic acid product, such as a wart paint, gel, or medicated plaster (commonly containing 17 - 50% salicylic acid).
They can also advise on safe application frequency, duration, and when to review progress — usually after 4 - 6 weeks of continuous treatment.
Avoid unregulated “natural” acid remedies or DIY freezing kits, as these can irritate or scar the skin.

At-home management (8–12 weeks)
Topical Salicylic Acid Treatment for Warts
The British National Formulary (2025) and NICE Clinical Knowledge Summaries (2024) recommend topical salicylic acid as a first-line treatment for common and plantar warts.
Salicylic acid (17–50%) regimen
-
Soak the wart in warm water for 5 - 10 minutes to soften the skin.
-
Gently file the surface with an emery board or pumice stone.
-
Protect the surrounding healthy skin with petroleum jelly or a barrier cream.
-
Apply the salicylic acid solution, gel, or plaster directly to the wart and allow it to dry.
-
Cover with a plaster or duct tape overnight.
-
Repeat once daily/ every other day for 8–12 weeks, or as advised by your pharmacist or clinician.
-
Pause treatment if the area becomes sore, inflamed, or bleeds.
-
With consistent use, up to 70% of warts clear (Gibbs et al., 2002; Kwok et al., 2012).
Frequency of use
-
Soaking: Soak the affected area once daily / every other day for 5 - 10 minutes in warm (not hot) water before applying the treatment. This softens the keratin layer and helps the acid penetrate more effectively.
-
Application: Apply topical salicylic acid once daily, ideally in the evening, after soaking and filing the wart. Let it dry fully before covering with a plaster or occlusive tape overnight.
When home treatments don’t work, I provide evidence-based procedures performed safely and hygienically, following NICE (2024) and BNF (2025) guidance.
In-clinic treatment options at odNOVA Aesthetics
1. Cryotherapy (Liquid Nitrogen)
Liquid nitrogen freezes infected keratinocytes and provokes immune clearance.
-
Frequency: every 2 - 3 weeks for 3 - 6 sessions.
-
Clearance rate: 50 - 70 % (Sterling et al., 2014).
-
Effects: transient pain, blistering or mild pigmentation change.
2. High-strength keratolytics
Prescription-grade salicylic acid 15 - 50 %, sometimes combined with urea, used to thin the wart and enhance immune exposure (British National Formulary, 2025; Kwok et al., 2012).
3. Chemical cautery (Trichloroacetic acid 50 - 80 %)
TCA chemically coagulates viral tissue for controlled exfoliation.
-
Indicated for: thick, resistant lesions.
-
Success: 60 - 80 % (Lipke, 2006; J Cutaneous Aesthetic Surg.)
-
Effects: mild redness or pigment change.
4. Curettage ± Electrocautery
Mechanical removal followed by cauterisation of the base.
-
Clearance: 70 - 80 % (Sterling et al., 2014).
-
Benefit: immediate removal; ideal for solitary warts.
-
Risks: minimal scarring with precise technique.
5. Immunotherapy (intralesional antigen injection)
NOT AVAILABLE
6. Plasma-Pen ablation
A medical plasma device sublimates tissue through controlled ionisation.
-
Ideal for: small, cosmetic warts.
7. Microwave therapy
NOT AVAILABLE
I provide clear aftercare instructions, discuss expected healing times and potential side-effects, and monitor progress until complete resolution. Most patients notice visible improvement within 4 - 8 weeks and full clearance within three months.
Summary and Prevetion
Key takeaways
-
Warts and verrucas are viral but benign.
-
They spread through direct contact, not poor hygiene.
-
Most will clear naturally, though treatment speeds resolution.
-
Professional care ensures safe, effective removal with minimal recurrence.
Long-term prevention
-
Keep skin hydrated and intact - cracks allow viral entry.
-
Avoid biting nails or picking at skin.
-
Wear flip-flops in communal areas.
-
Replace or disinfect pumice stones and footwear used during treatment.
-
Support immunity with adequate rest, nutrition and exercise.
My philosophy

1. Clinical assessment — focused history, dermoscopy, photography as needed.
2. Treatment plan — method, risks, scarring expectations, downtime, aftercare.
3. Procedure — local anaesthetic if required; precise removal using the least‑scarring technique for your lesion and location.
4. Aftercare & review — written instructions, 14‑day review; histology results if sent.
Typical appointment length: 20 - 40 minutes for simple removals.
FAQ:
1. Why do some people keep getting warts while others never do?
The difference lies in each person’s immune response. HPV is extremely common, but only a subset of people’s immune systems fail to recognise and destroy it effectively. Genetic factors, stress, sleep deprivation, poor nutrition, and immunosuppressive medication can all reduce viral clearance (Horn et al., 2005). Strengthening general immunity - through adequate rest, balanced diet, and reduced stress - can help prevent recurrence.
Can warts come back after they’ve been treated?
Yes, recurrence can occur even after successful removal. This happens when small amounts of virus remain in nearby skin or when there’s re-exposure from communal areas. Studies show recurrence rates vary from 10 - 30%, depending on the method used (Sterling et al., 2014; Lipke, 2006). Combining topical salicylic acid after in-clinic treatment and keeping skin intact reduces the likelihood of return.
Is it safe to swim or go to the gym if I have a verruca?
Yes — as long as it’s covered with a waterproof plaster or verruca sock. HPV spreads most easily in moist, communal environments such as swimming pool decks, showers, and changing rooms (NICE, 2024). Avoid walking barefoot, and disinfect flip-flops or gym shoes regularly.
Can shaving over a wart make it worse?
Absolutely. Shaving or waxing over a wart can micro-spread the virus to other follicles and surrounding skin, resulting in multiple new lesions. Always use separate razors or avoid shaving near affected areas until they are fully healed.
How are warts treated in children or those with sensitive skin?
In children, treatment is often gentler because their immune systems are naturally more likely to clear the virus. I usually recommend low-strength acid, soft occlusion therapy, and patience - most clear spontaneously within 6 - 12 months (Gibbs et al., 2002). Aggressive paring or freezing is avoided in younger patients to prevent pain or scarring.
References